HealthChoice inpatient rate changes proposed
Posted On: 1/22/2014
The Employees Group Insurance Division (EGID) of Oklahoma’s Office of Management and Enterprise Services (OMES) will hold a public meeting at 10 a.m., Wednesday, Feb. 12, for discussion of proposed inpatient hospital facility reimbursement rates for HealthChoice and Department of Corrections facilities, to be effective June 1, 2014.
EGID convened a task force of hospitals and the Oklahoma Hospital Association in October 2013 to get reactions to their proposals for rate changes. The proposals had been developed by EGID and their consultant, Berkeley Research Group. After receiving comments from the task force members in November, EGID presented modified proposals to the task force in December and the task force again commented. The proposal posted on Jan. 21 as part of the public hearing notice is the result of this consultative process.
The HealthChoice rate recommendations are grouped into four categories of change.
Issue 1 – Urban/Rural Distinction. HealthChoice now classifies hospitals as either urban or rural for payment rate purposes. The proposal establishes instead four tiers:
Tier 1 – Network urban facilities with greater than 300 beds
Tier 2 – All other urban and non-network facilities
Tier 3 – Critical Access Hospitals (CAH), Sole Community Hospitals (SCH), Indian, Military and VA facilities
Tier 4 – All other network rural facilities
Annual updates to the base rate:
Tier 1 and Tier 2 – 100 percent of Medicare’s full market basket percentage. (No productivity, ACA, etc., reductions)
Tier 3 – 50 percent of Medicare’s full market basket
Tier 4 – Remain frozen
Tier 3 and Tier 4 base rates will be reevaluated annually.
Issue 2 – Urban non-outlier claims. Recommendation:
Tier 1 – 13 percent increase in the base rate
Tier 2 – 5 percent increase in the base rate
Issue 3 – Neonatal. Recommendation: pay 70 percent of billed charges for MS-DRGs 789-794 to providers in all four tiers. MS-DRG 795 (normal newborn) will be paid the allowable rate per the MS-DRG fee schedule.
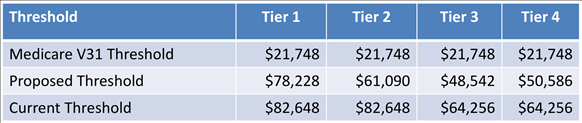
Issue 4 – Outliers. Recommendation:
- Establish thresholds for each tier based upon Medicare’s current IPPS impact file average Operating CCR and Capital CCR for Oklahoma network providers and Medicare’s published threshold.
- Establish a phase-in period for the marginal factor.
- The threshold will be updated each year with implementation of a new MS-DRG version.
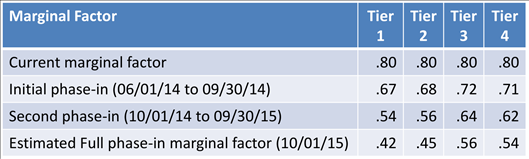

EGID’s rationale for the changes and additional supporting information, including their estimates of impact on Oklahoma hospitals, is linked in the
meeting notice.
Details of EGID’s proposed changes for Inpatient Reimbursement.
(Rick Snyder)